Occupational health risk management in construction: A guide to the key issues of occupational health provision
Summary Statement
This document was prepared by the Construction Industry Advisory Committee (CONIAC) Health Risks Working Group, which advises the Health and Safety Executive (HSE) of the UK on the protection of people at work. This guidance is aimed primarily at employers, but health and safety professionals and worker representatives should find it useful, too. It deals with health issues in construction, which are often given less focus than safety issues. It covers the following topics:
- what ‘health risk management’ means
- the roles in managing health risks at work
- what employers might need to do to comply with the law
- when an occupational health service provider might be needed and what you can expect from them
- the benefits to businesses and their workers of a well managed,
skilled occupational health service
- what health surveillance is and when you need to carry it
out.
July 2015
This document, prepared by the Construction Industry Advisory Committee (CONIAC) Health Risks Working Group, offers advice on assessing the risks to health in the construction industry and the role of occupational health service provision in preventing or controlling those risks. It's aimed primarily at employers, but others, such as directors, health and safety professionals, safety representatives and occupational health service providers, may find it useful, particularly in identifying their roles in the management of occupational health risks in construction.
July 2015
The guidance aims to help you understand:
- what 'health risk management' means
- the roles in managing health risks at work
- what you might need to do to comply with the law
- when you might need an occupational health service provider and what you can expect from them
- the benefits to businesses and their workers of a wellmanaged, skilled occupational health service
- what health surveillance is and when you need to carry it out.
CONTENTS
CONIAC Health Risks Working Group position on health risks in construction1. Defining occupational ill health
2. Occupational health risks in construction
3. How to assess the risks to workers
4. What is occupational health risk management?
5. Worker involvement and consultation
6. Hiring an occupational health service provider
7. What kind of occupational health provision?
8. Types of health surveillance
9. Asking the right questions when buying occupational health services
10. Making sure providers can carry out the occupational health services you want
11. What to expect from an occupational health service provider
12. What to do about restrictions on certain workers' exposures
13. Once I'm happy that I have a competent provider, that's my job done - right?
14. What if I have more than one occupational health service provider?
15. What about other health promotion and fitness-for-work programmes - how do they fit in?
Appendices
Glossary
CONIAC Health Risks Working Group position on health risks in construction
The Construction Industry Advisory Committee (CONIAC) advises the Health and Safety Executive (HSE) on the protection of people at work and others from hazards to health and safety within the building, civil engineering and engineering construction industries.
CONIAC's membership is tripartite - drawn from the HSE, employers and employees - and provides representation from key industry stakeholders, including small and medium-sized enterprises. The Chair of CONIAC is the Chief Inspector of Construction. CONIAC has four sub groups helping to take forward its work, including a Health Risks Working Group.
A position statement has been agreed and adopted by the CONIAC Health Risks Working Group, setting out its stance on managing health issues in construction.
- Workplace ill health kills and ruins lives in the construction industry. Statistics indicate that a construction worker is at least 100 times more likely to die from a disease caused or made worse by their work as they are from a fatal accident.
- Managing workplace health helps employers to retain experienced and skilled workers, and it helps employees to maintain productive employment.
- Workplace ill health is preventable - it is possible and practicable to carry out construction work without causing ill health. Risks to health can be managed by modifying the process to eliminate the risk, controlling and minimising exposure, and taking precautions to prevent adverse effects.
- Everyone involved in construction has a responsibility in managing risks to health, and all parties must take ownership of their part of the process.
- Planning and working collaboratively will reduce risk throughout the supply chain, and at all stages of the process. Workers and their representatives must be consulted regarding the provision of occupational health services and material occupational health issues.
- Managing health risks is no different to managing safety risks. Assessing hazards and using a hierarchy of control measures are equally appropriate when applied to health risks.
- Checking workers' health is not a substitute for managing and controlling health risks. Monitoring should not be given priority over managing, or be confused with it.
- Helping workers tackle other 'lifestyle' risks to their health is not a substitute for managing workplace health risks.
1. Defining occupational ill health
Occupational ill health refers to all health problems in the work environment. The term covers health problems workers bring to the workplace, as well as health issues caused or made worse by work. It covers serious and fatal diseases, physical effects on skin, breathing, hearing, mobility and functioning, and psychological effects on mental wellbeing. Effects may be immediate and visible, but are more often unseen and take a long time to develop, so vigilance and monitoring can be key to identifying problems. Some effects can be cured if diagnosed early; many can only be prevented from getting worse. Of course, some diseases are terminal.
There's a lot of confusion as to what 'occupational health' means. So, when speaking with others, you need to be clear on what they mean by the term.
This guidance provides advice on conditions caused or made worse by work; it does not cover the management of health problems that workers can bring to the workplace, eg diabetes, epilepsy. You can get more information on these issues at www.hse.gov.uk/disability.
2. Occupational health risks in construction
In construction, there are many dangers that can harm your workers. By law, you must eliminate, prevent or control the risks. Key risks include:
- exposure to asbestos, dusts including silica and lead, chemicals, sunlight, diesel engine exhaust emissions
- frequent loud noise
- frequent or excessive use of vibrating tools
- frequent or excessive manual handling of loads
- stress and fatigue.
For more information, visit www.hse.gov.uk/construction/healthrisks.
3. How to assess the risks to workers
Managing health risks is no different from managing safety risks. Thinking about what you do, how the risks cause harm and what you can do to prevent or control them are equally appropriate when applied to health risks.
This is known as risk assessment and it is something you are required by law to carry out. Risk assessment is about identifying and taking sensible and proportionate measures to control the risks in your workplace, not about creating huge amounts of paperwork. You are probably already taking steps to protect your employees, but your risk assessment will help you decide whether you should be doing more.
Think about how ill health could happen and concentrate on real risks - those that are most likely and which will cause the most harm. The following might help:
- consider your workplace activities, processes and the substances used that could harm employee health
- ask your employees what they think the hazards are, as they may notice things that are not obvious to you and may have some good ideas on how to control the risks
- check manufacturers' instructions or data sheets for chemicals and equipment, as they can be very helpful in spelling out the hazards
- some workers may have particular requirements, for example new and young workers, migrant workers, people with disabilities, temporary workers, subcontractors and lone workers.
The risk management cycle
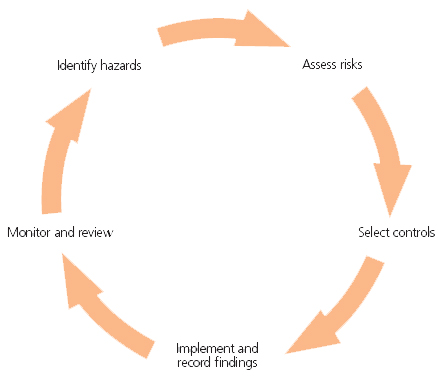
Having identified the hazards, you then have to decide how likely it is that harm will occur. Risk is a part of everyday life and you are not expected to eliminate all risks. What you must do is make sure you know about the main risks and the things you need to do to manage them responsibly. Generally, you need to do everything that is reasonably practicable to protect people from harm.
Make a record of your significant findings - the hazards, how people might be harmed by them and what you have in place to control the risks. Any record produced should be simple and focused on controls. If you have fewer than five employees you do not have to write anything down. But it is useful to do this so you can review it at a later date, for example if something changes. If you have five or more employees, you are required by law to write it down.
Few workplaces stay the same, so it makes sense to review what you are doing on an ongoing basis.
More guidance on risk assessment can be found at www.hse.gov.uk/risk.
In short...
You should look at all the potential dangers around your site and the work carried out, and then assess which workers are likely to be exposed to them. You should consider the hazard, the length of time workers are exposed and how much they're exposed to. If you're not sure what to do about health risks, a good starting point may be to talk to your trade association. At some point, an occupational health professional, occupational hygienist or ergonomist may help you assess the risks and identify control measures.
4. What is occupational health risk management?
Occupational health risk management is about putting in place a system to manage the risk of ill health caused by work activities.
At times you may employ occupational health service providers or others - such as occupational hygienists or other health and safety professionals - to give you advice and to help you manage any residual health risks once control measures have been introduced to reduce risks. Managing occupational health service provision is crucial to ensure all parties involved work together effectively to successfully manage risks to the health of your workers.
Taking an integrated view of all the health checks for workers can have benefits. For example:
- workers may feel more valued and, in turn, more motivated to keep fit to carry out their jobs
- encouraging workers to look after their health and wellbeing to improve their quality of life and life expectancy is likely to have an impact on their attitudes and behaviours towards workplace health risks
- speaking with workers about their general health and wellbeing, or about their fitness to do their job, provides an opportunity to coach and influence regarding workplace risks.
5. Worker involvement and consultation
Workplaces where employees are involved in taking decisions about their health are safer and healthier. Collaboration with your employees helps you to manage health risks in a practical way by:
- helping you spot workplace risks
- making sure health risk controls are practical
- increasing the level of commitment to working in a safe and healthy way.
You must consult all your employees, in good time, on health risk matters. In workplaces where a trade union is recognised, this will be through union health and safety representatives. In non-unionised workplaces, you can consult either directly or through other elected representatives.
Consultation involves employers not only giving information to employees but also listening to them and taking account of what they say before making decisions on managing health risks.
Issues you should consult employees on include:
- risks arising from their work
- proposals to manage or control these risks
- the best ways of providing information and training.
For more information on your legal duties, see the HSE leaflet Consulting employees on health and safety: a brief guide to the law (www.hse.gov.uk/pubns/indg232.htm). For more information on consulting with your employees, visit www.hse.gov.uk/involvement.
Where workplace controls and any health surveillance are required, they are more likely to be successful if workers understand what they are for and how they will benefit them. Experience in the industry has also shown that providing general health and wellbeing screening and initiatives in the workplace can improve buy-in and acceptance of health surveillance to help support the management of health risks. Workers focused on looking after their own health will often be more alert to the causes of ill health on site. Be clear, of course, of what is legally required and that general health and wellbeing initiatives are not a replacement for managing workplace health risks.
6. Hiring an occupational health service provider
If you decide you need help from an occupational health service provider, as with any other service you contract-out, you will want to make sure you get the right help. When recruiting their services, you should ensure they understand your workplace and workers. They should then be able to help you prioritise what you must, should and possibly like to do. However, you should understand the different types of health check and be clear about what you want the provider to do.
7. What kind of occupational health provision?
A traffic light system is a useful way of considering the variety of occupational health services available and can help you decide what is suitable and relevant for your workers and the tasks they perform.
- What must be done to ensure I comply with the law? - Red
- What could the provider do so that I can ensure the workers I have are fit, and remain so, to safely carry out the tasks required of them? - Amber
- What other health screening programmes would I like this service provider to deliver to promote worker involvement in reducing their risks of developing ill health? - Green
Table 1 outlines a simple approach to prioritising your requirements.
| Priority | Types of check | Examples |
| Red You must fully consider all options to eliminate health risks or control them to a minimum Where health risk remains, health surveillance is appropriate to help identify what more must be done to prevent harm and protect employees |
Legal requirements based on risk Health surveillance There are also other health checks required by driving licence law |
|
| Amber Industry accepted practice |
'Fitness for task' health checks for safety-critical tasks |
|
| Green Further checks to monitor the health of workers |
Health screening |
|
8. Types of occupational health surveillance
There are general legal duties to provide health surveillance under overarching health and safety legislation (Management of Health and Safety at Work Regulations 1999).
Periodic health surveillance is also required under specific laws, such as the Control of Substances Hazardous to Health Regulations 2002 (Regulation 11) and Control of Noise at Work Regulations 2005, which define what action needs to be taken at various exposure levels.
Under certain circumstances, by law you may need the services of an 'appointed doctor' to conduct statutory medical surveillance, eg for lead and asbestos.
9. Asking the right questions when buying occupational health services
If you require a level of an occupational health service provision to meet your legal duty, there are many factors you will need to agree and it may be useful to formalise these as service level agreements or key performance indicators.
Key points to note are whether the provider:
- has the skills, knowledge, experience and organisational capability to carry out the work you require of them. This will include those accredited with, for example, the Safe Effective Quality Occupational Health Service (SEQOHS) or Constructing Better Health (CBH)
- understands the nature of the work, workers and work environment.
To make sure you get a service that's fit for purpose, you should:
- share your risk assessments with them and any other relevant health and safety information
- allow them time to observe your workers and the work they do.
When setting up occupational health surveillance, you should consider what to do if a worker becomes ill and is no longer fit to perform their job, or if restrictions are put in place on what they can do. Can alternative work arrangements be made? Can tasks be rotated to reduce exposure? Your occupational health service provider should be able to assist you with these issues.
Implementing occupational health surveillance is a part of risk management. Where it is required, it is essential to get results fed back to verify whether your controls are successfully managing the health risks on site. It is also useful to get workers and their representatives involved in a health surveillance programme to feed back on how well they feel the risks are being managed.
10. Making sure providers can carry out the occupational health services you want
When looking to appoint occupational health service providers to undertake health surveillance, it is important to identify those who have the organisational capability to do so, eg those who have experience of working with the construction industry and a knowledge of the risks. A medical professional may not always be required - a trained responsible person, for example, could take charge of surveying the workforce for early signs of ill health. Table 2 provides brief descriptions of key roles in occupational health service provision. More information on the specific standards needed can be found on the HSE website at http://www.hse.gov.uk/health-surveillance/index.htm.
| Title | Description | Qualifications to look for |
| Appointed doctor | Doctor approved by the HSE to undertake statutory health checks under certain regulations, eg for asbestos and lead | The HSE website holds a list of appointed doctors in your area - go to www.hse.gov.uk/doctors |
| Occupational health physician or occupational health nurse | Medical professional, with specific occupational health qualifications, who provides health surveillance, eg for noise and hand-arm vibration Levels of qualifications can be confirmed with the appropriate governing body |
Physicians: General Medical Council, Faculty of Occupational Medicine
|
| Occupational hygienist | Professional trained to recognise, evaluate and control risks associated with hazardous substances, such as asbestos, cement and silica | Certificate of Competence awarded by the British Occupational Hygiene Society |
| Occupational health technician | Professional trained and qualified in specific areas, such as spirometry and audiometry Technicians should be under the supervision of qualified occupational health physicians or nurses |
Relevant certificates and diplomas for levels of qualification/training |
| Responsible person | Someone given responsibility to help deliver a system of occupational health surveillance, eg administering screening questionnaires for hand-arm vibration, asthma and skin inspections for dermatitis The role will be clearly defined. It will be a person trusted by the workforce, with good communication and interpersonal skills. If ill health is observed, an appropriately qualified doctor or nurse must be consulted |
Evidence of training/coaching on what they need to do in order to perform their role effectively May be trained by health professional, management, health and safety professional or other, as appropriate |
Do I always need a doctor or nurse?
No. In many cases there are things you can do to keep costs down by putting a trained 'responsible person' in charge of surveying the workforce for early signs of ill health. However, you will still need to call on appropriately qualified (competent) professionals to deal with any ill health. If you have a large workforce, it's worth having a competent occupational health professional contracted or employed to be in charge of your programme to advise and assist you in managing health risks.
11. What to expect from an occupational health service provider
Agree with your provider what feedback is appropriate. As a minimum, obtain regular anonymised feedback of the results of health surveillance in a way that allows you to see if workers' health is being affected by work activities. This will help you review your systems of work and controls as part of your risk management duties.
You must also receive information for each worker undergoing health surveillance regarding their 'fitness' for continued exposure to particular hazards at work, as well as any limitations or restrictions. You should receive certificates for those workers undergoing 'fitness for task' checks.
12. What to do about restrictions on certain workers' exposures or tasks
Your occupational health service provider will use their professional judgement to provide you with advice on future restrictions on exposures at work and the fitness of individuals to continue working with certain exposures. You should already have considered what you might do if this situation comes up. However, you can always talk it through with your occupational health service provider and consider the advice they give. There are duties under the Equality Act 2010 which require you to assess the need for appropriate adaptations to the work and workplace, wherever it would be considered reasonable to do so. There are also rules under the Reporting of Injuries, Diseases and Dangerous Occurrences Regulations 2013 to report certain diseases associated with particular tasks.
'Fitness for task' checks
This is the process whereby individuals are assessed against a set of standards to ensure they are capable of safely undertaking the tasks involved in their job role and are not a risk to themselves or others. The focus of these checks is to enable workers to work safely and productively.
Some fitness for task assessments are legal requirements (eg HGV medical), industry requirements (eg personal trackside safety (PTS) when working in or around railways), or recommended practice (eg safety-critical workers). Where there are no specific legal or industry guidelines for the fitness for task for a particular job role, the employer and the occupational health service provider should decide on the content and scope of the assessment in line with good practice and/or be evidence based, eg Constructing Better Health's 'Health assessment matrix'. In all cases, the checks should be carried out in consultation with the workers and their representatives.
An important factor in fitness for task assessments is the Equality Act 2010, which ensures that people classified as having a disability should not be discriminated against in the workplace.
Medical confidentiality
Your occupational health service provider must protect confidential medical information contained in medical records. If medical details are disclosed to you following written consent, you must retain the medical information but separate it from the health record. This is because the medical information is confidential to the employee and is not to be disclosed to a third party.
13. Once I'm happy that I have a competent provider, that's my job done - right?
No. You should continue to manage the control of risks to health, including the occupational health service provision. This involves monitoring and reviewing the performance of the controls you have in place. Reviewing and analysing the results of occupational health checks will assist in this.
You should act on any advice given by your occupational health service provider. Meeting and talking at regular intervals with your occupational health service provider, as well as any other professionals involved, will help ensure you're successfully managing health risks on site. You must also keep health records for all those undergoing occupational health surveillance.
Health records
The employer has a duty to keep health records for all workers undergoing health surveillance.
These are different to medical records, which contain confidential medical information, and are kept by the occupational health service provider.
Workers' health records contain general information such as name, date of birth, employee number, and also relevant exposure information with the outcome of any health surveillance in relation to their fitness for task. An example of a health record is given in Appendix 3.
Health records should be kept for as long as the worker is under health surveillance. For work relating to hazardous substances and asbestos, records should be kept for 40 years. For work involving ionising radiation, it's 50 years. It's helpful to give workers their health records when they leave your employment to take to their next employer, although you should keep copies for future reference. They should not contain medically confidential information about an individual. Under the Data Protection Act 1998, you have to inform employees that you have a health record for them, and that they have a right to access that information and correct it.
14. What if I have more than one occupational health service provider?
This situation can be common and can make the management of occupational health risks more difficult. Good channels of communication between you and all the providers, as well as between the providers, will ensure consistency and that relevant information is shared.
15. What about other health and wellbeing and fitness-for-work programmes - how do they fit in?
General health and wellbeing services offer a two-fold benefit: they can encourage the promotion of better health among workers whose lifestyles make health a challenge; and workers concentrating on better health for themselves will often be more alert to the causes of ill health on site. However, any wellbeing initiative should not be seen as a substitute for managing the workplace risks themselves and will be most effective if integrated with the risk management arrangements, eg a smoking cessation programme alongside a targeted initiative on reducing respiratory risk from silica exposure.
Appendices
Appendix 1: Top tips for putting occupational health service arrangements in place
Item |
Check |
| Prioritise your occupational health service needs (the 'red, amber, green' approach can simplify this) | |
| Agree this with your provider | |
| Check your provider has the organisational capability to carry out the tasks you require of them | |
| Agree roles, responsibilities and what communication you both need and expect | |
| Agree the format and frequency of tests and feedback of results, particularly from occupational health surveillance | |
| Agree the procedures and roles for referring workers with ill health for diagnosis or further treatment | |
| Agree and set up systems for maintaining appropriate records, particularly health records | |
| Consider options to deal with workers who are in ill health and who may no longer be fit for their current position or need to have adjustments made | |
| Set up a system to act on the results you receive from health surveillance tests | |
| Agree a timescale for reviewing the occupational service and its performance in helping you manage the risks of ill health at work | |
| At appropriate stages, consult your workers and their representatives on issues that will affect them, and inform them of which health checks are required and why |
Make sure you don't lose sight of the hazards to health you are exposing workers to. However, having a workforce interested in looking after its health is likely to bring benefits not only to the workers themselves but also to the business through:
- workers being present at work, not off sick
- workers being fit and healthy to perform the work required of them
- increased productivity
- safer working practices and fewer accidents.
Remember: a happier, healthier workforce makes good business sense.
Appendix 2: Useful links
- HSE advice on carrying out risk assessments www.hse.gov.uk/pubns/indg163.pdf
- HSE advice on managing health risks in construction www.hse.gov.uk/construction/healthrisks
- HSE advice on health surveillance requirements www.hse.gov.uk/health-surveillance
- Help with finding an appropriate occupational health provider
Constructing Better Health can provide a list of accredited providers www.cbhscheme.com, as well as guidance on topics such as drug and alcohol testing
The Commercial Occupational Health Providers Association can help source an appropriate occupational health provider www.cohpa.co.uk - Help with finding an occupational hygienist and how they can help advise on the recognition, evaluation and control of workplace health risks www.bohs.org
- Faculty of Occupational Medicine's guidance on Safe Effective Quality Occupational Health Service (set of standards and voluntary accreditation to help raise the standard of care provided by occupational health services) www.seqohs.org
- To check the registration of occupational physicians, visit www.gmc-uk.org
- To check the registration of an occupational health nurse, visit www.nmc-uk.org
- HSE information on medical surveillance for appointed doctors www.hse.gov.uk/doctors/index.htm
- HSE advice on reporting occupational disease under RIDDOR www.hse.gov.uk/riddor/what-must-i-report.htm#occupational
- Home Office advice on duties under the Equality Act www.homeoffice.gov.uk/equalities/equality-act
- Strategic Forum for Construction. Medical fitness to operate construction plant www.cpa.uk.net/sfpsgpublications/#MedicalFitness
- Driver and Vehicle Licensing Agency. At a glance guide to the current medical standards of fitness to drive www.gov.uk/government/uploads/system/uploads/attachment_data/file/418165/aagv1.pdf
Appendix 3: Example of health record
| Name of organisation: | ||||||
| Surname | Forename(s) | Gender | ||||
| Permanent address |
Postcode |
National Insurance Number
| Date when present employment started | |||
| Historical record of jobs in this employment involving exposure to identified substances requiring health surveillance |
||||||
| Results of health surveillance | ||||||
| Date carried out | Reason for health surveillance | Who undertook health surveillance? | Outcome (fit/not fit/ fit with restrictions) | Additional comments | Health surveillance review date | |
Glossary
Biological monitoring
Methods used to measure and assess uptake and/or effects of exposure to substances, eg by testing blood, urine or breath samples.
Duty holder
An employer with specific duties to their workers under statutory health and safety requirements.
Fitness for task
Checks to ensure the person employed is and remains fit to carry out particular tasks without risk to themselves or others. Results of health screening tests may be checked against a set of standards to be met for particular tasks, eg for a forklift truck driver.
Health monitoring
A system of checking workers' health on a regular basis where the risks to health and their effects are recognised but the evidence base is not so well developed, and/or there are no validated techniques to measure them.
Health records (see Appendix 3)
Records relating to individuals under health surveillance that must be held by the employer. They should be differentiated from the confidential medical records generated and held by the occupational health service provider undertaking health surveillance. They contain information on the individual, where they work, the hazards they've been exposed to and dates in relation to this. They also detail the outcome of health surveillance and an employee's fitness to continue working with exposure to certain hazards.
Health risk management
Preventing workers from suffering adverse effects on their health caused by their job, by avoiding or controlling risks through task and worker adaptation.
Health screening
A specific test or tests for particular health problems, such as blood pressure or diabetes. May be done as part of a 'fitness for task' assessment.
Health surveillance
A statutory risk-based system of ongoing health checks required when workers are exposed to hazardous substances or activities that may cause them harm. It helps employers to regularly monitor and check for early signs of work-related ill health in these employees.
Medical confidentiality
The ethical principle and legal right that a doctor or other health professional will hold secret all information relating to a patient, unless the patient gives disclosure consent.
Medical surveillance
A type of health surveillance for highhazard exposures that often involves clinical examination and may include specific tests that must be under the control of an appointed doctor with appropriate training and experience. The term is specifically referred to in a number of regulations, such as those relating to lead, asbestos and hazardous substances.
Occupational hygiene
The professional discipline of recognising, evaluating and controlling risks to health in the workplace to prevent ill health.
Safety-critical worker
Any person who, if incapacitated during the course of their task, has the potential to cause a significant safety risk to others or, because of the environment in which the task is undertaken, puts themselves at significant risk of harm.
About the CONIAC Health Risks Working Group
The Health and Safety Executive's Construction Industry Advisory Committee includes a number of groups with specialist remits. The Health Risks Working Group is made up of a wide range of construction industry representatives. The following members of the Working Group have contributed to this guide:
| Ian Strudley (Chair) - Health and Safety Executive | Marianne Dyer - Consultant Occupational Physician |
| Jacquie Brown (Secretariat) – Health and Safety Executive | Kevin Fear - Construction Industry Training Board |
| Clare Forshaw – Health and Safety Executive | Melodie Gilbert - Park Health and Safety Partnership |
| David Ackerley - IOSH Construction Group | Caroline Haslam - Home Builders Federation |
| Michelle Aldous - Constructing Better Health | Kevin Minton - Construction Plant Hire Association |
| Paul Bussey - Royal Institute of British Architects | Susan Murray - Unite |
| Denis Doody - Union of Construction, Allied Trades and Technicians | Gren Tipper - Construction Clients Group |
| Andy Turrell - UK Contractors Group |
The Group acknowledges the support of IOSH in publishing and hosting this guide to occupational health in construction. The document joins IOSH's range of authoritative, free guidance, available at www.iosh.co.uk/techguide.
IOSH
The Grange
Highfield Drive
Wigston, Leicestershire
LE18 1NN
UK

IOSH is the Chartered body for health and safety professionals. With more than 44,000 members in over 120 countries, we're the world's largest professional health and safety organisation.
We set standards, and support, develop and connect our members with resources, guidance, events and training. We're the voice of the profession, and campaign on issues that affect millions of working people.
IOSH was founded in 1945 and is a registered charity with international NGO status.


Institution of Occupational Safety and Health
Founded 1945
Incorporated by Royal Charter 2003
Registered charity 1096790
t+44 (0)116 257 3100
www.iosh.co.uk
twitter.com/IOSH_tweets
facebook.com/IOSHUK
tinyurl.com/IOSH-linkedin
POL1271/210715/PDF


