Summary Statement
This PowerPoint from a presentation at a 2012 CPWR meeting by Carrie Redlich MD reviews the
main findings of a NIOSH-funded study looking at health effects from exposure to spray polyurethane foam as part of green construction. The results point out the strong relationship between this work and occupational asthma and addresses
the medical evaluations needed. Case studies are presented of workers who developed sensitivity.
March 27, 2012
Exposure to “Green” Polyurethane Spray Foam
- What’s in it
- Potential health effects ‐ isocyanate asthma
- Challenges
- Biomonitoring ‐ Isocyanate-specific IgG / IgE
- CPWR study – preliminary data
- Questions
Chemical Composition of SPF
- Methylene diphenyl diisocyanate (MDI) /pMDI
- Polyols (petroleum or soy based)
- Amine catalysts
- Flame retardants
- Blowing agents
- Surfactants
Part A – Isocyanates
Part B – variable / proprietary
Mix A + B = POLYURETHANE FOAM
(exothermic reaction)
Major Commercial Isocyanates
HDI - hexamethylene
- O=C=N(CH2)6N=C=O
Paints, Coatings Light resistant
TDI - toluene
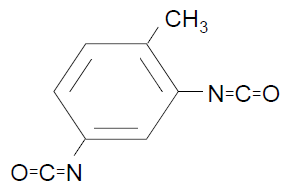
MDI - diphenylmethane or methylene diphenyl
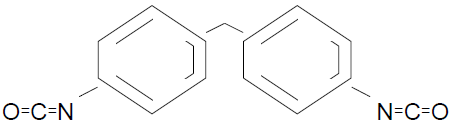
Less volatile – “safe”
Foams, adhesives Coatings, wood products
Uses Isocyanates / Polyurethanes in Construction - Growing
- Foams – soft / hard
- Insulation – spray foam
- Simulated wood – doors, posts
- Adhesives
- Roofing materials
- Caulking
- Sealants
- Elastomers / coatings
- Woodbinder – composite wood
Health Effects Isocyanates
- Potent sensitizer / allergen
- Occupational asthma
- One of the most commonly identified causes of occupational asthma
- Rash / skin irritation - less common, but occurs
- Hypersensitivity pneumonitis – less common.
Isocyanate asthma – key features
- Clinically similar to “ordinary” asthma
- Timing- onset months to years after onset exposure
- Delayed symptoms 6-8 hours after exposure
- Once sensitized, exposures to very low levels trigger asthma
- Diagnosis can be missed – (by patient and doctor)
- Asthma commonly persists after away from exposure
- Poor socioeconomic outcomes – unemployment, reduced income
- Extent problem unknown – especially in end-user settings
Health effects from exposure to other components PU Foam ?
- Amine catalysts
- Sensitizers, irritants – asthma, rash
- Blurry vision (halo vision)
- Flame retardants
- VOCs
- Blowing agents
- Polyols
Routes of exposure / forms
- Inhalation
- Skin – likely contributes to sensitization and asthma
- Liquid, aerosol, vapor
- Exothermic reaction
- Cut & shave foam → dust, particulates
Case
Healthy 36 y/old construction worker / insulator 1 yr ago started use PU spray foam. Past 5 months -‐ cough after work / evening – wife concerned. Chest tightness, SOB, wheeze. Better on weekends. Symptoms progress – goes to ER.
Initial Medical evaluation
No h/o asthma, allergies. Improves with asthma inhalers. Continues to work, wears PPE, but progressive symptoms.
Further work‐up
Spirometry – airflow obstruction ‐ positive BD response MDI‐IgG, MDI‐IgE positive. Told to avoid isocyanates.
Health Effects of Exposure to “Green” Polyurethane Spray Foam
- What’s in it
- Potential health effects ‐ isocyanate asthma
- Major challenges
- Biomonitoring ‐ Isocyanate ‐specific IgG / IgE
- CPWR study – preliminary data
- Questions
Limitations isocyanate exposure assessment and regulation
- Multiple formulations and forms– vapor / aerosol / particulates
- Sampling and laboratory analysis can be challenging
- All methods depend on free NCO – timing critical
- “Snapshot” of exposure ‐ end‐user settings esp problematic
- Air sampling does not assess effectiveness personal protective equipment (gloves, respirator)
- Skin exposure assessment methods limited
- Current OELs – Not protective
Limitations diagnosis isocyanate asthma
- Asthma common condition ‐ connection to work frequently missed – especially once asthma more chronic.
- No simple specific test for isocyanate asthma. Frequently other work (and environmental) triggers.
- Most clinicians focus on treatment more than cause / prevention
- Worker may leave causative job / work before diagnosis made, but asthma frequently persists.
- No mandatory medical surveillance or reporting for isocyanate asthma
Biomonitoring Approaches
- Direct measurements of isocyanate derivative or metabolite in urine - currently not useful
- Measurements of physiologic response to exposure (antibodies in blood)
Principles Guiding Isocyanate Serology
Isocyanate chemicals are “man-made” - don’t exist naturally.
Humans don’t normally make antibodies to isocyanate modified albumin; they are triggered by exposure.
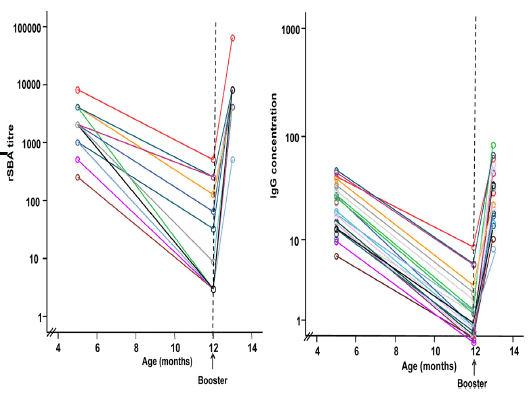
Without ongoing exposure, specific antibodies are cleared from blood in a time dependent manner.
Isocyanate Immunoassays
- Detect in human serum
- Isocyanate-specific IgG and IgE responses
- Integrated measurement over time
- IgG serum1/2 life = 30 days
- IgE serum 1/2 life ~ 2 days
- Response highly specific for isocyanate
- Can vary depending upon form of isocyanate used as the “antigen”
Measures human response to exposure
Biomonitoring hexamethylene diisocyanate (HDI) exposure based on serum levels of HDI-specific IgG
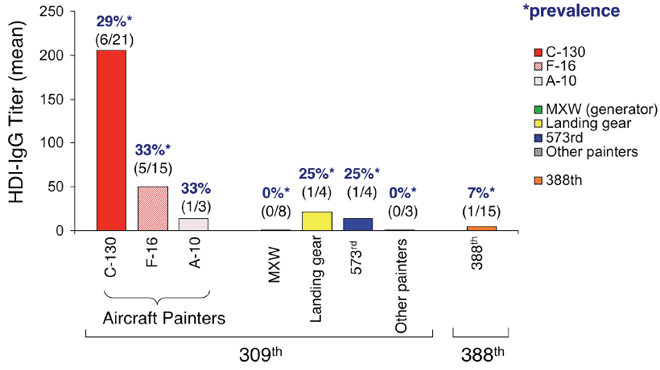
Wisnewski. Ann Occup Hyg 2012; 10: 1-10
Case: PU spray foam sprayer MDI-IgG over time
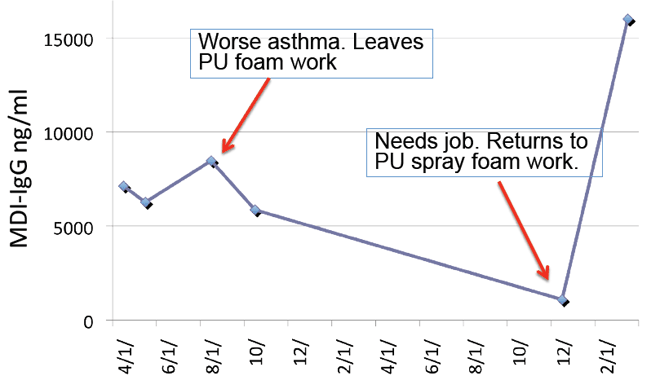
Assessment and Prevention of Isocyanate Exposures in the Construction Industry Funded by NIOSH / CPWR
Aim 1) Assess respiratory and skin isocyanate exposures in the construction industry
Aim 2) Implement a surveillance program for construction workers who work with or around PU products.
Aim 3) implement an intervention program to reduce isocyanate exposures in construction workers.
Characteristics Construction Workers Recruited who use Isocyanate Products (n= 60) Preliminary Data
| Gender: Male | 58 (97%) | ||
| Current smoker | 22 (37%) | ||
| Job Category | |||
| Insulator | 20 (33%) | ||
| Other | 40 (67%) | ||
| Glazier / taper | 9 (15%) | ||
| Energy conservation | 7 (12%) | ||
| Other construction | 24 (40%) | ||
| Symptoms | |||
| None | 19 (32%) | ||
| Non-specific | 24 (40%) | ||
| Asthma, work-related | 15 (25%) | ||
| Spirometry - airflow obstruction | 16 (27%) | ||
Worker Self Reported Exposure (n= 60) Preliminary Data
| Other spray near you | ||
| No | 7 (12%) | |
| Monthly or less | 14 (23%) | |
| Daily / weekly | 39 (65%) | |
| Get Isocyanate product on skin | ||
| Never | 4 (7%) | |
| Occasionally | 22 (37%) | |
| Frequently | 34 (57%) | |
| Where on skin | ||
| Hands, arms, wrists | 24 (40%) | |
| Head, neck, face | 15 (25%) | |
Work-related symptoms preliminary data (n = 60)
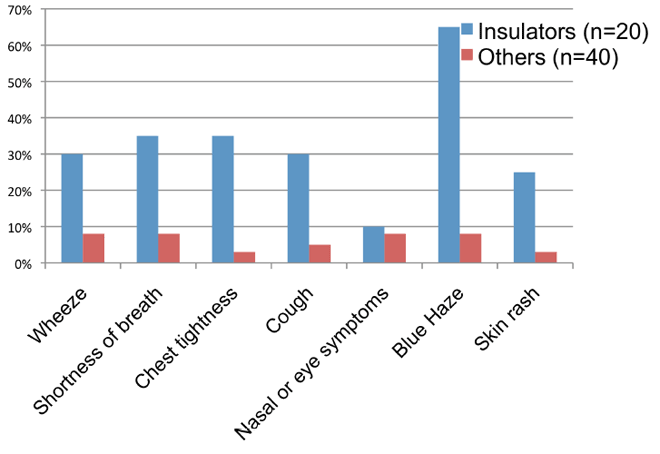
Possible Asthma: prior diagnosis vs study diagnosis preliminary data (n = 60)
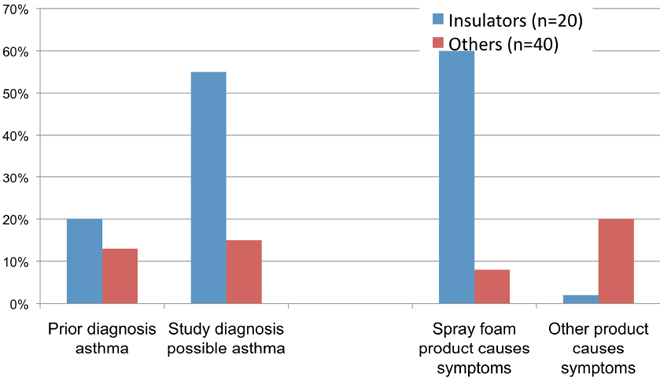
Prevalence of isocyanate-specific-IgG Comparison to autobody workers preliminary data
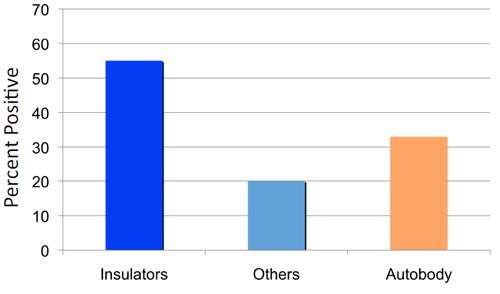
MDI specific-IgG titres (mean) preliminary data (n = 60)
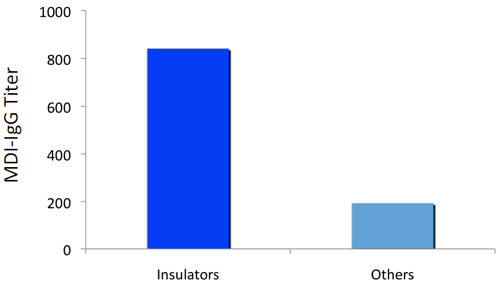
PU Construction Worker Project – Initial Preliminary Conclusions
- Work‐related asthma symptoms are common in the PU spray foam workers – may represent isocyanate asthma
- High prevalence MDI‐IgG positive titers in PU spray foam workers
- MDI skin exposure is commonly reported
- Traditional IH monitoring does not appear to be adequate
Health Effects of Exposure to “Green” Polyurethane Spray Foam
- What’s in it
- Potential health effects ‐ iIsocyanate asthma
- Major challenges
- Biomonitoring ‐ Isocyanate‐specific IgG / IgE
- CPWR study – preliminary data
- Questions
Acknowledgements
Yale Occupational and Environmental Medicine Program
Adam Wisnewski, PhD
Meredith Stowe, PhD
Judy Sparer, CIH
UMass
Dhimiter Bello, PhD
Funding
CPWR-NIOSH Construction Center Grant “Assessment and
Prevention of Isocyanate Exposures in the Construction Industry”


